Get Drug and Alcohol Rehab Covered at Icarus Nevada with Cigna Insurance
Seeking help for drug and alcohol addiction treatment is a tough decision that requires great courage and commitment. Most people struggle to make this decision because they find it difficult to admit that they may need professional help to deal with drug or alcohol addiction problems.
Discovering that drug rehab is beyond your reach because of financial constraints can be very demoralizing. People suffering from addiction often find themselves trying to find ways to cover the cost of regaining their overall well-being and health.
According to the Substance Abuse and Mental Health Service Administration (SAMHSA), about 23.5 million Americans over 12 years suffer from a substance use disorder. However, only about 10% seek and get addiction treatment. Don’t let financial concerns stop you or your loved one from getting effective recovery support!
At Icarus Behavioral Health in Nevada, we provide in-network Cigna drug rehab coverage for added convenience. Keep reading to learn more about getting drug and alcohol rehab covered at Icarus Nevada using with Cigna Insurance.
Does Cigna Cover Addiction Treatment in Nevada?
Cigna, a global health organization, covers its customers’ participation in substance abuse treatment programs. It has partnered with treatment centers for substance abuse to offer its members access to low-cost detox, inpatient residential, and outpatient programs.
Insurance companies are obligated by the Affordable Care Act (ACA) to provide treatment for mental health conditions, including substance use disorders like coverage for drug and alcohol addiction.
While insurance coverage varies based on your specific plan, addiction recovery treatment plans may include the following:
- Drug rehabilitation services
- Alcohol Rehab
- Medical detox
- Counseling and therapy for the treatment
Most Forms of Cigna Coverage Accepted – Call Now!
What Services Does Cigna Cover for Substance Abuse Treatment in Nevada?
Based on your plan, Cigna addiction treatment coverage with Icarus Nevada as an in-network provider may include the following services:
1. Medical Detox Services
In most cases, you may require assistance detoxing from drugs and alcohol, which can be uncomfortable, painful, or even life-threatening. Because of the constant medical monitoring provided by medical detox, withdrawal from drugs and alcohol can be made safely. You may also be prescribed medicine to help with the discomfort of withdrawal.
2. Inpatient Rehab Programs
Drug and alcohol treatment support is available at inpatient rehab or residential live-in treatment centers. The average time spent in an inpatient facility ranges from 15 to 90 days.
3. Partial Hospitalization Programs (PHP)
Living at home while receiving necessary medical care is made possible through partial hospitalization programs. These programs allow you to attend to other life commitments when receiving treatment.
4. Intensive Outpatient Program (IOP)
A few evenings each week are dedicated to attending treatment sessions in an intensive outpatient program. While participating in an IOP, you have the freedom to live at home and maintain your regular day-to-day responsibilities.
5. Outpatient Treatment
Individuals who have completed inpatient treatment typically attend outpatient treatment for continuous assistance on their journey to sobriety. You’ll spend most of your time at home, but go to a rehabilitation center for 10 to 12 hours per week for treatment and guidance.
The amount of addiction treatment costs Cigna members must pay for themselves varies based on the specific plan. The monthly premium, copayments, deductibles, and other fees may change from one plan to the next. However, with health insurance from Cigna, you can rest assured that at least some of your expenses will be covered.
Does Cigna Cover Inpatient Rehab in Nevada?
Cigna insurance plans usually cover at least some portion of residential rehab treatment. It is usually more expensive than outpatient rehab, but consider it an investment in your future. You may be entitled to the following services:
- Inpatient detoxification for a severe drug or alcohol addiction
- Partial hospitalization for alcohol or drug abuse
- Substance abuse treatment in an inpatient setting
Your insurance plan determines the out-of-pocket costs for residential rehab. Cigna provides the following insurance policies:
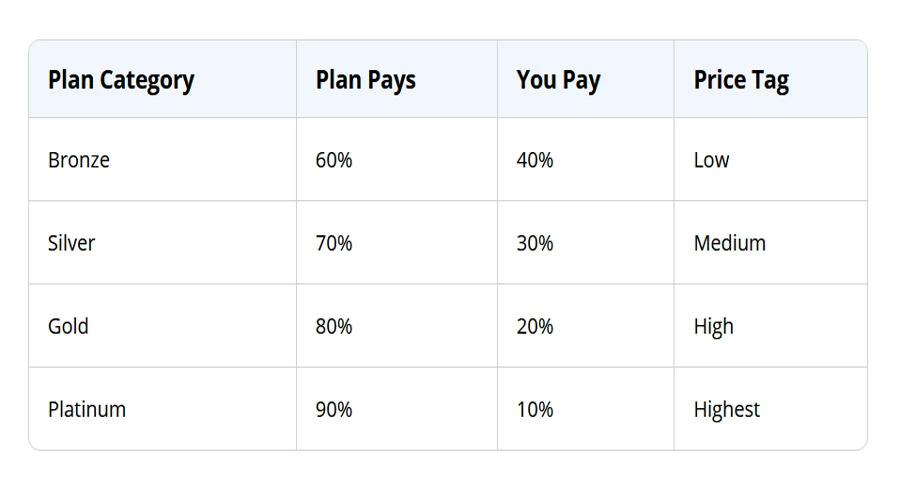
Platinum
After meeting the deductible, consumers with Cigna’s Platinum insurance plan should anticipate paying between 10% and 30% coinsurance. A Platinum plan will usually pay for some treatment at an out-of-network facility, based on your state of residence.
Gold
After you’ve paid the deductible, coinsurance for an in-network provider runs between 20% and 40%. Some policies will cover an out-of-network provider to some extent in some states. In other areas, however, you must only see a pre-vetted in-network treatment provider.
Silver
On a Cigna Silver plan, the coinsurance for an in-network treatment program is usually between 30% and 50% – but only after you satisfy the deductible. The availability of out-of-network amenities depends entirely on the state in which you live.
Bronze
Cigna’s Bronze plan usually only covers the charges after you’ve paid all your deductibles. Some policies will help cover out-of-network fees, but others will require you to pay the total amount.
Typical Cigna Outpatient Rehab Coverage With Various Plans
Below are the cost estimates for outpatient rehab services under Cigna Insurance:
- Bronze Plans: Coinsurance is determined by the state of residency and can range from 0% to 50%. These plans may or may not cover out-of-network care.
- Silver Plans: Several in-network outpatient services may have a coinsurance percentage, while others have a charge per visit. Out-of-network providers are either covered or not.
- Gold Plans: In-network patients may be required to pay a minor coinsurance percentage or a copay per visit, depending on the service offered. Out-of-network services are either covered or not.
- Platinum Plans: In-network providers have low coinsurance or payment requirements. Out-of-network insurance coverage is available under some policies. However, coinsurance rates are often higher for these procedures.
Cigna Health Insurance Coverage for Rehab: Typical Levels and Plans
Cigna Health plans fall into various categories and have different features based on the following:
- The state you live in
- Your employer (if you have obtained insurance through an employer)
- Qualification for government-funded healthcare like Medicaid and Medicare
- Whether you chose your plan through the Affordable Care Act (ACA) marketplace
The health plans under Cigna fall into different main categories, such as:
- Health Maintenance Organization (HMO): HMO plans are an excellent option for people comfortable with a limited number of health care providers within the Cigna network. These plans cover care provided by physicians and facilities in contracts with the insurance company.
- Exclusive Provider Organization (EPO): An EPO plan offers more flexibility to clients in selecting a doctor or facility for healthcare. However, some services are only accessible in in-network treatment centers.
- Preferred Provider Organization (PPO): PPO plans allow clients to choose from a broader range of healthcare providers for added convenience. However, getting care outside of the network leads to high out-of-pocket expenses.
Below are other options that Cigna provides:
- LocalPlus Plans: These affordable plans allow clients to receive healthcare services from a limited network.
- Open Access Plans (OAP): Although similar to a PPO Cigna health insurance plan, an OAP plan has a broader network of providers.
Free & Confidential Insurance Verification – Reach out Now!
What Does Cigna Cover for Substance Abuse Treatment in Nevada?
Your benefits and coverage will vary depending on your Cigna plan. For example, Cigna’s most basic plan, bronze, have lower premiums but higher deductibles and out-of-pocket payments. On the other hand, those with gold or platinum plans receive more extensive coverage with smaller deductibles.
Programs for substance abuse treatment are covered by insurance and the costs you will be responsible for vary substantially depending on the type of plan and the state you live in. Contact your health insurance provider to evaluate your policy and see whether therapy services are covered under your plan.
Must You Receive Treatment in an In-Network Facility?
While not all Cigna plans need your treatment center in-network, it is essential to understand that hiring an out-of-network physician typically raises your out-of-pocket payments.
Some plans may not cover out-of-network services, leaving you to foot the tab. Other plans will cover specific sections if a deductible or coinsurance has been met.
Pre-certification is required for several out-of-network treatment choices. Cigna will check the request against nationally accepted guidelines.
In circumstances where pre-certification is required, Cigna will assess which services are covered based on your plan. Icarus in Nevada proudly offers in-network Cigna status, and can verify your insurance details in minutes via confidential call.
Does Cigna Cover Rehabilitation in an Out-of-State Facility?
When looking for the right rehab center for yourself or a loved one, the choice between in-network and out-of-network institutions is one of the primary elements that will affect the cost and coverage of the treatment program. To keep costs down, make sure you choose a drug addiction physician with a contract with Cigna or an in-network provider such as Icarus.
If you opt to seek treatment outside of the state, coverage will depend on your insurance plan and its specifications. Cigna may be able to cover some of the costs of out-of-network treatment in some situations, but this would be much less than in an in-network treatment, though, as we’ve mentioned, Icarus Nevada is in-network with Cigna.
Our Proven Therapies and Other Treatment Options at Icarus Nevada
You learn all you need for long-term rehabilitation as part of your Cigna drug treatment coverage. This education encompasses addiction coping techniques, life skills, and relapse prevention.
Cigna drug rehab centers also offer individual counseling, group, and family therapy. These therapies assist you in understanding your addiction and avoiding a relapse into active substance abuse.
Behavioral therapies are among the most effective treatments provided by your Cigna drug rehab plan.
Cognitive Behavioral Therapy (CBT) assists you in changing negative thoughts and emotions while improving your behavior. CBT is an excellent tool for achieving and maintaining sober. It also helps you in improving other aspects of your life.
Dialectical Behavioral Therapy (DBT), like CBT, assists you in changing your behavior. This type of CBT aids in the treatment of mood disorders and other issues associated with addiction. DBT is a component of dual diagnosis treatment in a licensed rehabilitation facility. Dual diagnosis treatment assists you in recovering from your addiction as well as any related mental health issues.
These therapies and treatment methods are simply a sampling of the services provided by your Cigna drug rehab coverage. Consider yourself fortunate to have this policy and its perks since you require treatment for your addiction.
Up to 100% of Treatment Costs Covered with Cigna
Get Effective Support for Recovery Using Cigna at Icarus Nevada
Our drug rehab facilities in Nevada offer highly specialized drug addiction treatment and behavioral health services, all as an in-network Cigna provider. We offer a wide range of solutions for people seeking to recover from substance abuse and mental health disorders.
Call us today for a confidential consultation, and get treatment covered by Cigna insurance at Icarus in Nevada today!